
CGM and Diet: How 50+ Foods Affect Blood Sugar Differently
CGM data reveals how different foods, meals, and macronutrient combinations affect glucose — with 20-80 mg/dL post-meal variation between individuals for the same food.
Why Glucose Responses to Food Are Highly Individual
One of the most powerful insights from continuous glucose monitoring is that glucose responses to the same food vary dramatically between individuals. A landmark 2015 study published in Cell by Zeevi et al. at the Weizmann Institute tracked 800 participants with CGMs for a week and found that postmeal glucose responses to identical foods varied by up to 4-fold between individuals. One participant had a large glucose spike from bananas but not from cookies, while another showed the opposite pattern. The key factors driving individual variability include gut microbiome composition (the species and ratios of bacteria in your intestines), insulin sensitivity (how effectively your cells respond to insulin), genetic variations in glucose transporter proteins, meal timing relative to circadian rhythm, physical activity level, and sleep quality. This research shattered the one-size-fits-all approach to dietary advice and provided the scientific foundation for personalized nutrition guided by CGM data. A continuous glucose monitor is the only practical way to discover your individual glucose response to specific foods.
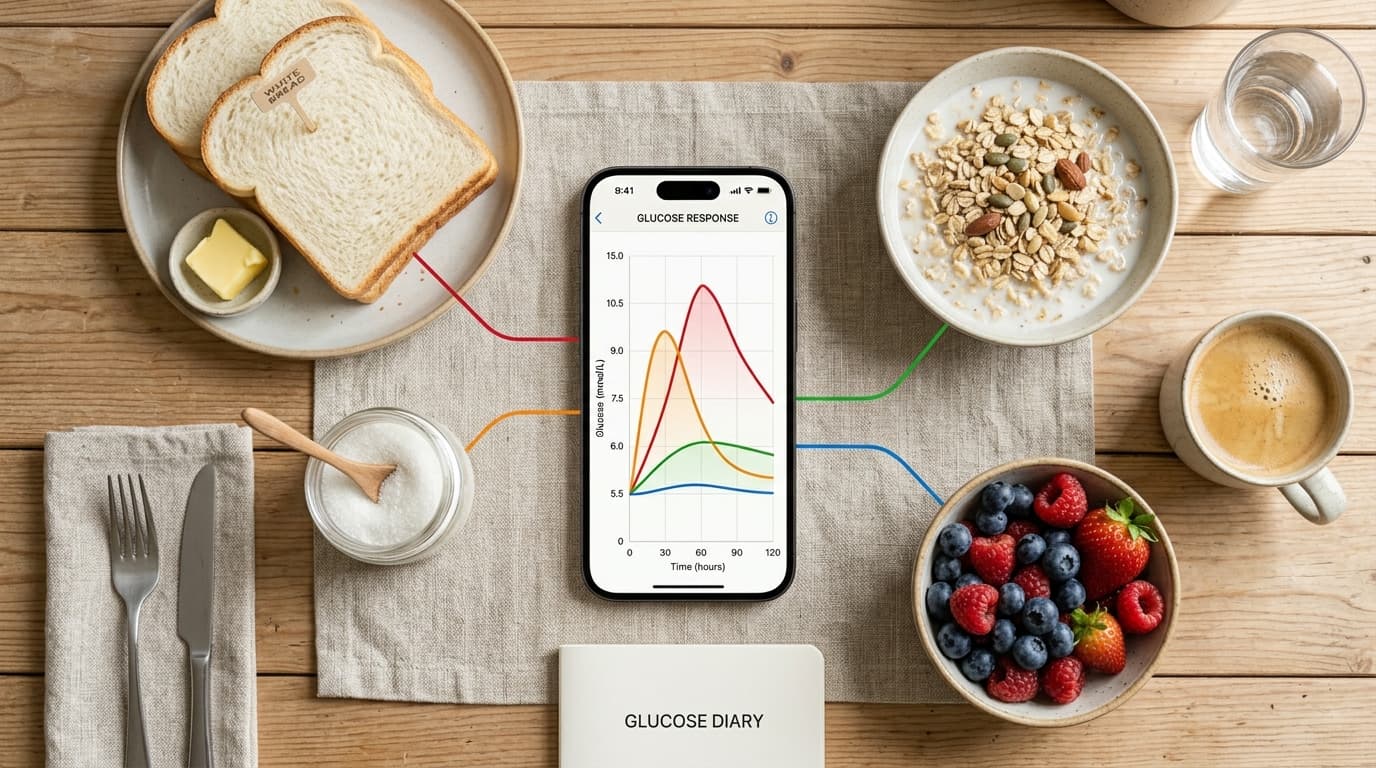
Foods That Commonly Spike Blood Sugar
While individual responses vary, certain food categories consistently produce large glucose spikes across most people. White bread, white rice, and refined pasta have glycemic indices above 70 and typically raise glucose by 40 to 80 mg/dL within 30 to 60 minutes. Fruit juices and smoothies deliver concentrated sugars without the fiber that slows absorption, often spiking glucose by 50 to 70 mg/dL. Breakfast cereals — even those marketed as healthy — frequently contain 15 to 25 grams of added sugar per serving. Potatoes (glycemic index 78 for baked russet) can spike glucose by 50+ mg/dL. Sweetened yogurts, granola bars, and "energy" snacks often produce larger spikes than their marketing suggests. On the other hand, many CGM users discover that certain high-carb foods cause surprisingly modest glucose responses for them personally — for example, sourdough bread typically produces a 20 to 30% smaller spike than white bread due to the organic acids produced during fermentation.
How Meal Composition Affects the Glucose Curve
The macronutrient composition of a meal matters as much as the carbohydrate content. Eating carbohydrates alone produces the fastest and tallest glucose spike. Adding protein reduces the spike by 20 to 30% because protein slows gastric emptying and stimulates insulin secretion independently of glucose. Adding fat further blunts the spike by an additional 10 to 15% through the same gastric emptying mechanism. The order in which you eat macronutrients also matters: a 2023 study in Diabetes Care demonstrated that eating vegetables and protein before starches reduced the peak glucose response by 35% compared to eating starches first. Fiber, particularly soluble fiber from sources like oats, beans, and psyllium, forms a gel-like matrix in the stomach that physically slows glucose absorption. Vinegar (1-2 tablespoons before a meal) reduces postmeal glucose peaks by 20 to 30% through an acetic acid mechanism that delays gastric emptying and increases muscle glucose uptake. These strategies are visible and verifiable through CGM data within a single meal.
Using CGM to Build a Personalized Diet
The practical approach to building a CGM-informed diet involves 3 phases. Phase 1 (Days 1-7): Eat your normal diet without changes and log every meal in your CGM app. This establishes your baseline and identifies your worst glucose offenders. Phase 2 (Days 8-21): Systematically test modifications to your top spike-causing meals — add protein, swap refined grains for whole grains, try different cooking methods, and experiment with meal order and timing. Track the glucose impact of each change. Phase 3 (Day 22+): Implement the changes that produced the best results and verify that your average glucose, time in range, and glucose variability metrics improve. Most users find that 5 to 8 dietary swaps account for 80% of the improvement. Common high-impact swaps include replacing white rice with cauliflower rice or brown rice, choosing sourdough bread over white bread, adding nuts or avocado to smoothies, eating a protein-rich breakfast instead of cereal, and moving the largest carbohydrate serving to lunch rather than dinner (when insulin sensitivity is typically highest).