Metabolic Syndrome: 5 Diagnostic Criteria and Cardiovascular Risk Factors
Metabolic syndrome requires 3 of 5 criteria: elevated waist, triglycerides, blood pressure, fasting glucose, or low HDL. Affects 35% of US adults. Diagnosis, IDF vs ATP III, cardiovascular risk, and management.
What Is Metabolic Syndrome?
Metabolic syndrome is a clinical diagnosis assigned when a person simultaneously meets 3 or more of 5 specific cardiometabolic criteria: elevated waist circumference, high triglycerides, low HDL cholesterol, high blood pressure, and elevated fasting glucose. It is not a single disease but a constellation of interconnected risk factors that, when clustered together, dramatically amplify the risk of cardiovascular disease, type 2 diabetes, stroke, and premature death. Approximately 35% of American adults — roughly 84 million people — meet the diagnostic threshold according to NHANES (National Health and Nutrition Examination Survey) data. Prevalence increases sharply with age: 20% of adults under 40, 35% of adults aged 40-59, and nearly 50% of adults over 60. The syndrome was first described by Gerald Reaven at Stanford University in 1988 as "Syndrome X," and the name was updated to "metabolic syndrome" by the National Cholesterol Education Program in 2001. The unifying pathophysiology behind all 5 criteria is insulin resistance — the inability of cells to respond normally to insulin — which drives elevated glucose, promotes hepatic triglyceride production, suppresses HDL synthesis, increases sodium retention (raising blood pressure), and promotes visceral fat accumulation.
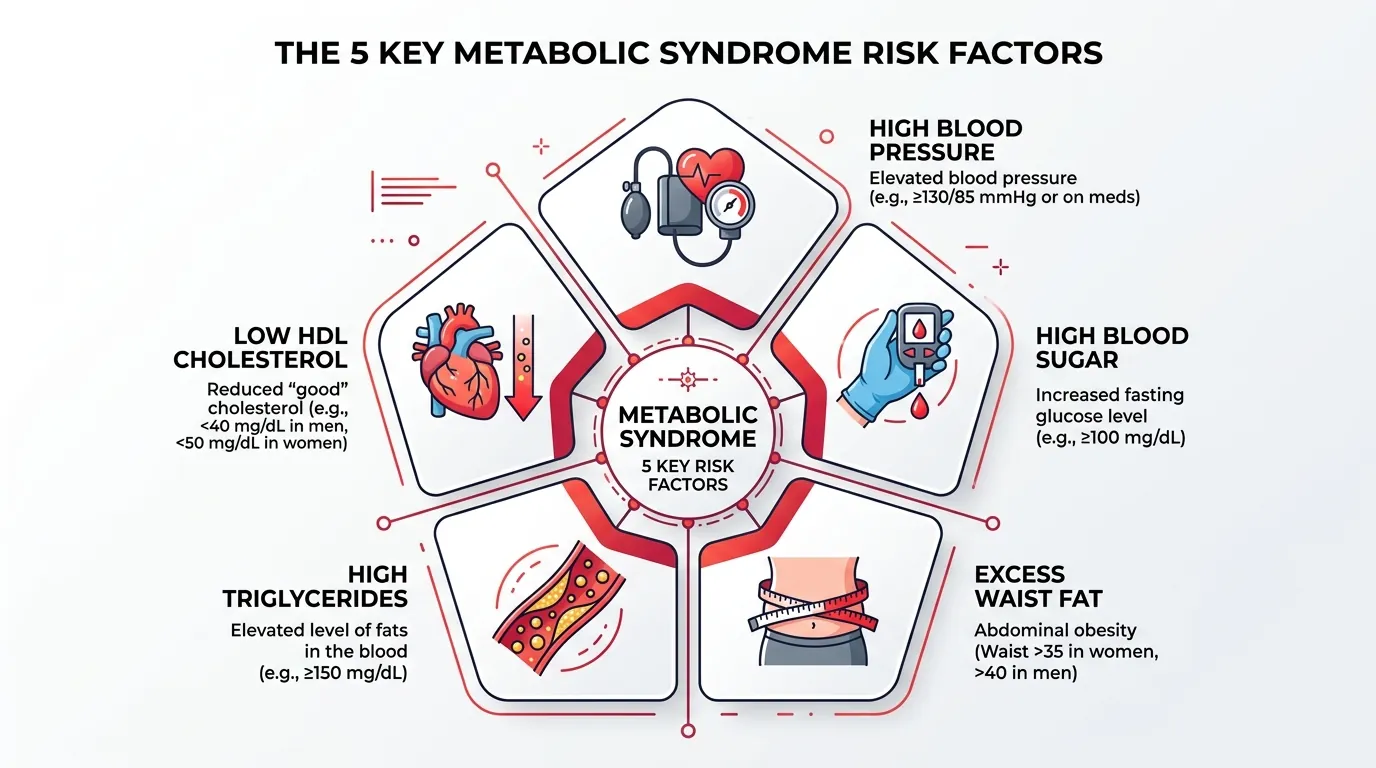
The 5 Diagnostic Criteria
A diagnosis of metabolic syndrome under the Adult Treatment Panel III (ATP III) criteria requires meeting 3 or more of the following 5 criteria, with no single criterion being mandatory: (1) Waist circumference greater than or equal to 40 inches (102 cm) in men or greater than or equal to 35 inches (88 cm) in women, measured at the level of the iliac crest. (2) Triglycerides greater than or equal to 150 mg/dL, or currently taking medication for elevated triglycerides. (3) HDL cholesterol less than 40 mg/dL in men or less than 50 mg/dL in women, or currently taking medication for low HDL. (4) Blood pressure greater than or equal to 130/85 mmHg, or currently taking antihypertensive medication. (5) Fasting glucose greater than or equal to 100 mg/dL, or currently taking medication for elevated glucose. The most common 3-criteria combination is elevated waist circumference + high triglycerides + low HDL, which accounts for approximately 40% of metabolic syndrome diagnoses. The least common combination involving elevated blood pressure + high fasting glucose + low HDL (without central obesity) suggests a primarily hepatic insulin resistance pattern rather than a visceral fat-driven pattern.
IDF vs ATP III: Two Competing Diagnostic Frameworks
Two major organizations have published competing diagnostic criteria for metabolic syndrome, and the differences matter clinically. The ATP III criteria (National Heart, Lung, and Blood Institute, 2001; updated 2005) use the 5-criteria model described above with equal weighting — any 3 of 5 qualifies. The International Diabetes Federation (IDF) criteria (2005) require central obesity (elevated waist circumference) as a mandatory prerequisite, plus 2 of the remaining 4 criteria. The IDF also uses lower, ethnicity-specific waist circumference thresholds: greater than or equal to 94 cm for European men, greater than or equal to 80 cm for European women, greater than or equal to 90 cm for South Asian, Chinese, and Japanese men, and greater than or equal to 80 cm for South Asian, Chinese, and Japanese women. Under IDF criteria, a person with high triglycerides, low HDL, and elevated glucose — but normal waist circumference — would not be diagnosed with metabolic syndrome, even though they meet 3 of 5 ATP III criteria. In U.S. clinical practice, most physicians use the ATP III criteria, which identify a slightly broader population. A 2015 meta-analysis in Diabetes Care found that both frameworks predicted cardiovascular events with similar accuracy (hazard ratio 1.53 for ATP III vs 1.49 for IDF), so the choice of framework has minimal impact on risk stratification.
Cardiovascular Risk: The Numbers
Metabolic syndrome roughly doubles the 10-year risk of cardiovascular events and increases the risk of type 2 diabetes 5-fold compared to metabolically healthy individuals. A 2016 meta-analysis in the Journal of the American Heart Association analyzing 87 studies with 951,083 participants quantified the excess risk: coronary heart disease increased by 99% (hazard ratio 1.99), stroke by 46% (HR 1.46), cardiovascular mortality by 68% (HR 1.68), and all-cause mortality by 47% (HR 1.47). The risk is synergistic — the combination of 3+ metabolic abnormalities produces greater cardiovascular damage than the sum of each individual factor. Each additional failed criterion beyond 3 adds approximately 10-15% to 10-year mortality risk. A 2017 analysis of 942,366 participants in the Journal of the American College of Cardiology showed that individuals with all 5 criteria had a 59% higher all-cause mortality rate compared to those meeting zero criteria. For type 2 diabetes specifically, the San Antonio Heart Study followed 2,815 non-diabetic adults for 7.5 years and found that metabolic syndrome at baseline predicted diabetes conversion with 53% sensitivity and 84% specificity — meaning metabolic syndrome correctly identified more than half of future diabetes cases.
Managing Metabolic Syndrome
First-line treatment for metabolic syndrome is comprehensive lifestyle modification targeting all 5 criteria simultaneously. The Diabetes Prevention Program demonstrated that 150 minutes per week of moderate exercise combined with 5-7% body weight loss reduced diabetes risk by 58% and improved all metabolic markers. Specific interventions by criterion: for waist circumference, caloric restriction targeting 500-750 kcal/day deficit produces 1-2 pounds of weight loss per week, with visceral fat preferentially mobilized during the first 10% of weight loss. For triglycerides, reducing refined carbohydrates and alcohol while increasing omega-3 fatty acids (2-4 grams EPA/DHA daily) can reduce triglycerides by 25-50%. For HDL, aerobic exercise raises HDL by 3-9% over 8-12 weeks; quitting smoking raises HDL by 5-10% within 3 months. For blood pressure, the DASH diet reduces systolic pressure by 8-14 mmHg; sodium restriction below 2,300 mg/day provides additional 2-8 mmHg reduction. For fasting glucose, the dietary and exercise changes described above typically normalize fasting glucose within 8-12 weeks if insulin resistance is the primary driver. When lifestyle modification is insufficient after 3-6 months, pharmacological intervention targets individual criteria: statins or fibrates for lipids, ACE inhibitors or ARBs for blood pressure, and metformin for elevated glucose. CGM-guided nutrition — using real-time glucose data to identify personal food sensitivities — provides an additional 25-35% improvement in postmeal glucose control beyond standard dietary counseling according to a 2020 Nature Medicine trial.