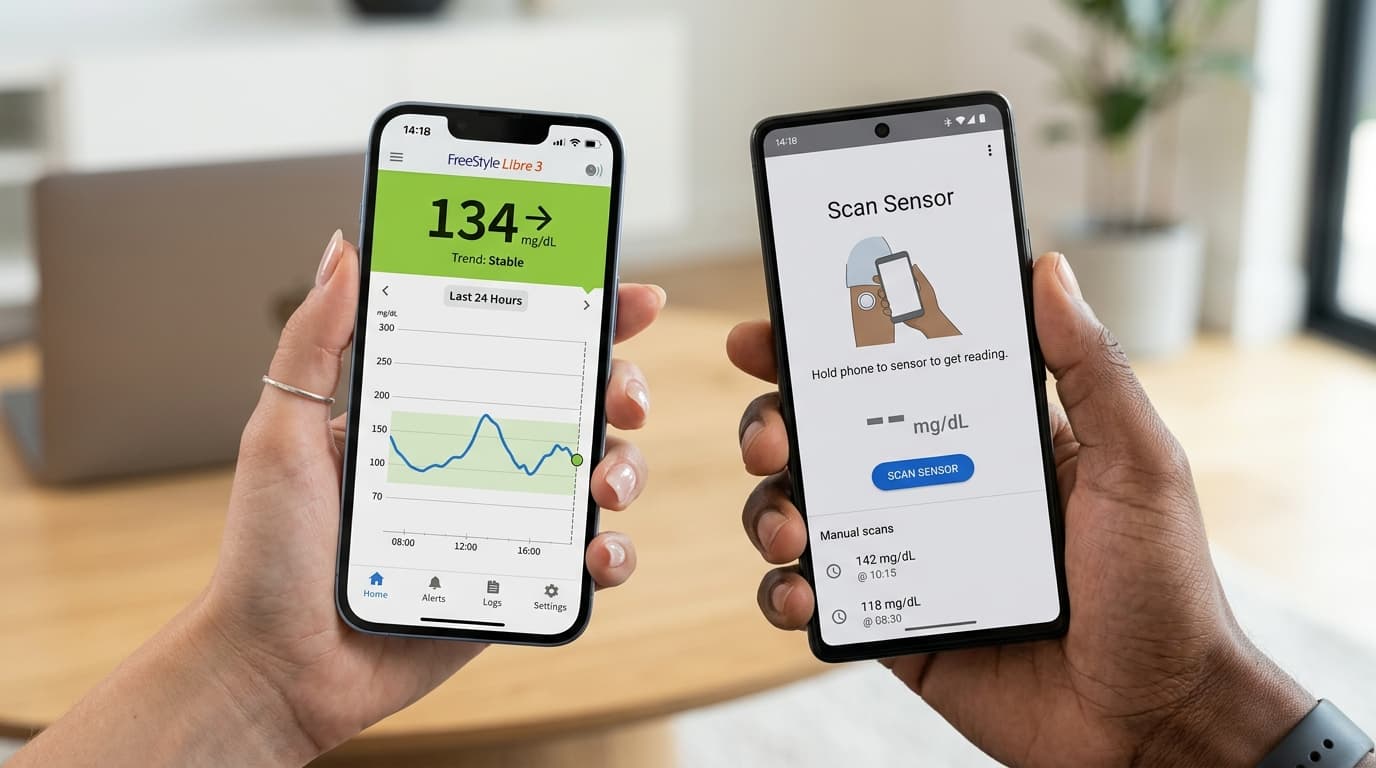
Real-Time CGM vs Flash Monitoring: Continuous Data vs On-Demand Scans
Real-time CGMs push readings every 1-5 minutes with alerts. Flash monitors require manual scans. The clinical and practical differences explained for glucose monitoring.
Two Categories of Continuous Glucose Monitoring
Continuous glucose monitors fall into two categories based on how they deliver data to the user: real-time CGM (RT-CGM) and flash glucose monitoring (FGM), also called intermittently scanned CGM (isCGM). Real-time CGMs automatically transmit glucose readings to a paired device every 1 to 5 minutes without any action from the user. Flash glucose monitors store data on the sensor and display the current reading only when the user actively scans the sensor with a smartphone or dedicated reader. This distinction matters clinically because real-time devices can deliver proactive high and low glucose alerts, while flash monitors only show alarms if the user happens to scan during an out-of-range event. The gap between these two categories has narrowed significantly — the FreeStyle Libre 3 transitioned from flash to real-time monitoring — but understanding the difference remains important when choosing a device.
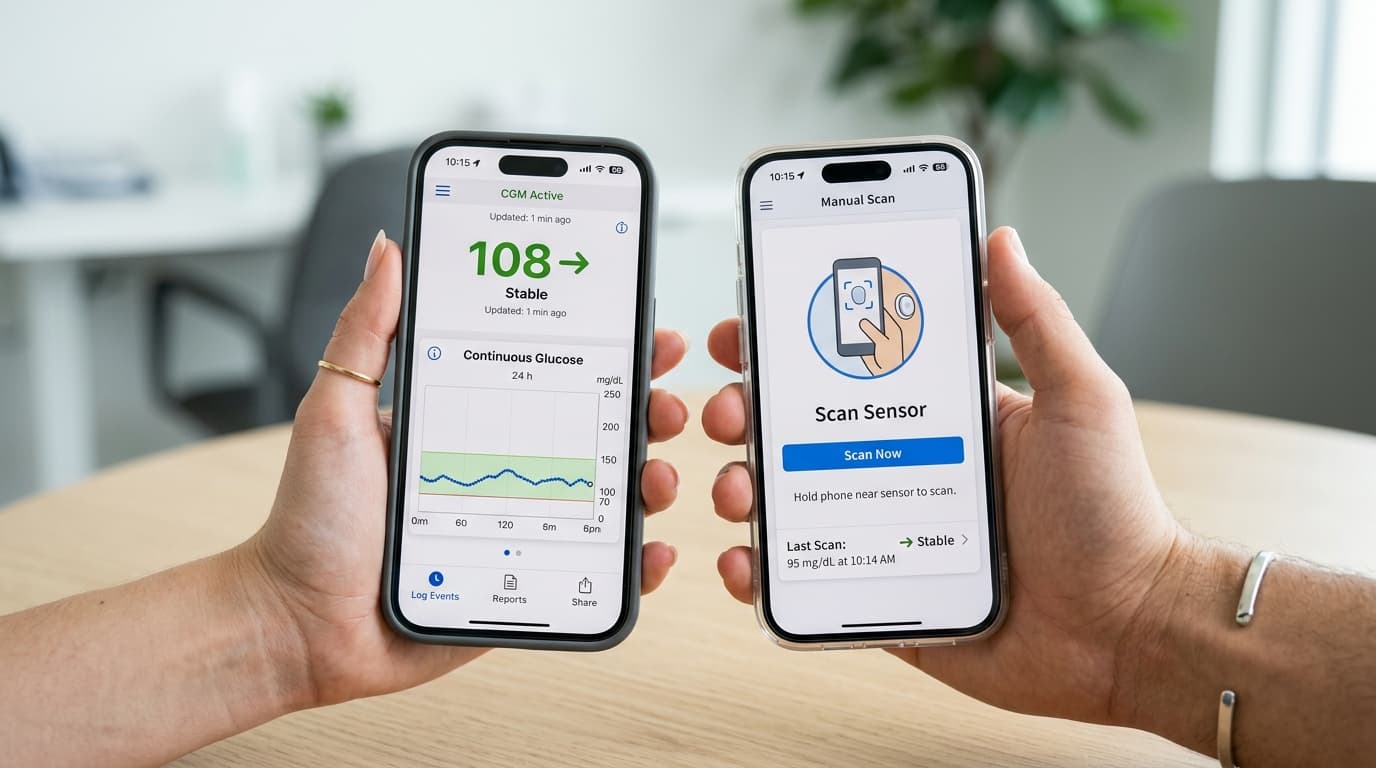
How Real-Time CGM Works
Real-time CGMs maintain a continuous Bluetooth connection between the on-body transmitter and the paired smartphone, smartwatch, or insulin pump. Every 1 to 5 minutes, the transmitter pushes a new glucose reading to the display device without requiring any user interaction. If the phone moves out of Bluetooth range (typically 6 to 10 meters), the sensor continues storing readings internally and backfills the data when the connection is restored. The defining feature of real-time CGM is proactive alerting: users can set customizable thresholds for high glucose (e.g., above 180 mg/dL), low glucose (e.g., below 70 mg/dL), and rate-of-change alerts that warn when glucose is rising or falling rapidly. The Dexcom G7, FreeStyle Libre 3 Plus, and Eversense E3 are all classified as real-time CGMs. For people on insulin therapy, real-time alerts reduce severe hypoglycemic events by up to 72% according to the HypoDE trial published in The Lancet.
How Flash Glucose Monitoring Works
Flash glucose monitors record glucose data continuously to the sensor's internal memory but do not transmit readings automatically. To see the current glucose value and recent trend data, the user must hold a smartphone or dedicated reader near the sensor (within 1 to 4 centimeters) to perform a near-field communication (NFC) scan. The scan retrieves the current reading plus up to 8 hours of stored trend data. If the user does not scan for more than 8 hours, the oldest data is overwritten and lost. The Abbott FreeStyle Libre 2 was the most prominent flash glucose monitor, and it offered optional alarms that could alert users when scanned readings fell outside preset thresholds — but these alarms required the sensor to be within range and were not as reliable as true real-time alerts. As of 2026, Abbott has largely transitioned its product line to real-time monitoring with the Libre 3 and Libre 3 Plus, but the Libre 2 remains available in some markets.
Choosing Between Real-Time and Flash CGM
For most users, real-time CGM is the superior choice. The proactive alerts prevent dangerous glucose excursions, especially overnight and during exercise when manual scanning is impractical. Real-time CGM is essential for anyone on insulin therapy, anyone with hypoglycemia unawareness, and anyone using a closed-loop insulin pump system (which requires continuous data input). Flash monitoring may still be appropriate for cost-conscious users with type 2 diabetes on oral medications only, where the risk of severe hypoglycemia is low and the primary goal is learning glucose patterns after meals. The price difference has narrowed substantially: as of 2026, real-time CGMs like the FreeStyle Libre 3 cost approximately the same as the older flash-based Libre 2, making the clinical case for flash monitoring increasingly difficult to justify.