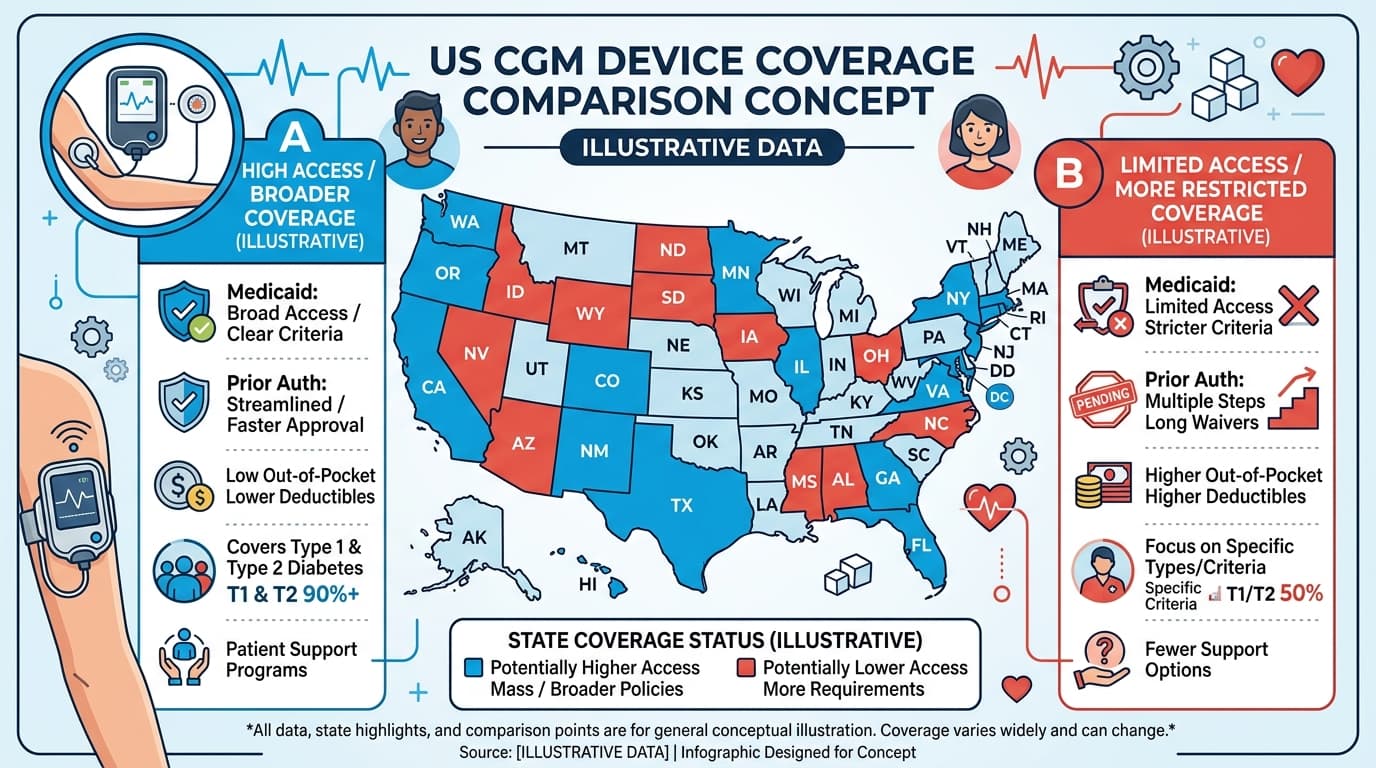
Medicaid CGM Coverage by State: 2026 Guide
Medicaid CGM Coverage Overview
Medicaid coverage for continuous glucose monitors varies by state because each state administers its own Medicaid program with individual coverage policies. As of 2026, the majority of state Medicaid programs cover CGMs for patients with type 1 diabetes on insulin therapy. Coverage for type 2 diabetes patients is less uniform — approximately 35 states cover CGMs for insulin-treated T2D, while some states require additional clinical criteria such as hypoglycemia unawareness or documented A1C above a threshold. Medicaid managed care plans within each state may have additional coverage nuances beyond the state fee-for-service policy.
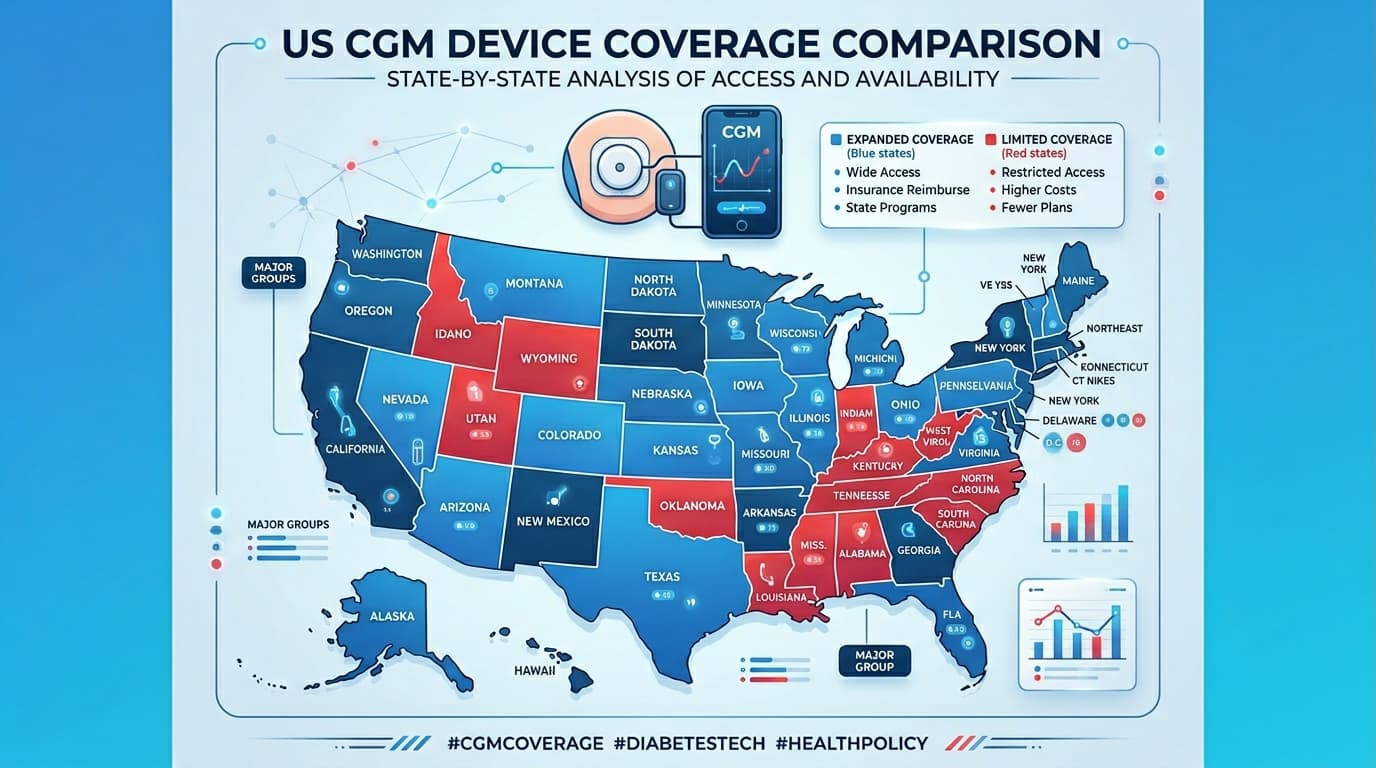
Covered Devices and Limitations
Most state Medicaid programs that cover CGMs approve the FreeStyle Libre 3 Plus and Dexcom G7 as preferred devices due to their established clinical evidence and cost-effectiveness. Some states designate one brand as preferred (requiring step therapy before approving the other), while others allow physician choice. The Medtronic Guardian 4 is generally covered when prescribed as part of a Medtronic MiniMed 780G pump system. Implantable CGMs (Eversense) are rarely covered by Medicaid. Over-the-counter CGMs are not covered by any state Medicaid program.
How to Access CGM Through Medicaid
Patients should start by asking their endocrinologist or primary care physician to prescribe a CGM and submit a prior authorization request to the state Medicaid program or managed care plan. Prior authorization requirements typically include documentation of insulin use, a diabetes diagnosis, and a statement of medical necessity. If coverage is denied, patients have the right to file an appeal — Medicaid fair hearing processes are available in every state. Advocacy organizations such as the American Diabetes Association and JDRF provide free assistance with Medicaid CGM coverage appeals.
How to Check Your State's Medicaid CGM Coverage
Medicaid CGM coverage varies by state because each state administers its own Medicaid program with different formularies and prior authorization requirements. To check your state's coverage: (1) call your Medicaid managed care plan's pharmacy or DME department, (2) ask specifically about CGM coverage under both pharmacy and DME benefits — some states cover CGMs under one but not the other, (3) request the prior authorization criteria so your physician can submit documentation that meets your state's specific requirements. Currently, approximately 38 states cover at least one CGM brand for Medicaid enrollees with type 1 diabetes, while coverage for type 2 diabetes varies more widely.