Blood Sugar Testing Methods Compared: CGM vs Fingerstick vs Lab A1C
CGM provides 288 daily readings at 7.9-9.1% MARD. Fingersticks give 4-10 readings at +/-15%. Lab A1C offers one 3-month average. Full comparison of accuracy, frequency, cost, and clinical use.
Overview of Blood Sugar Testing Technologies
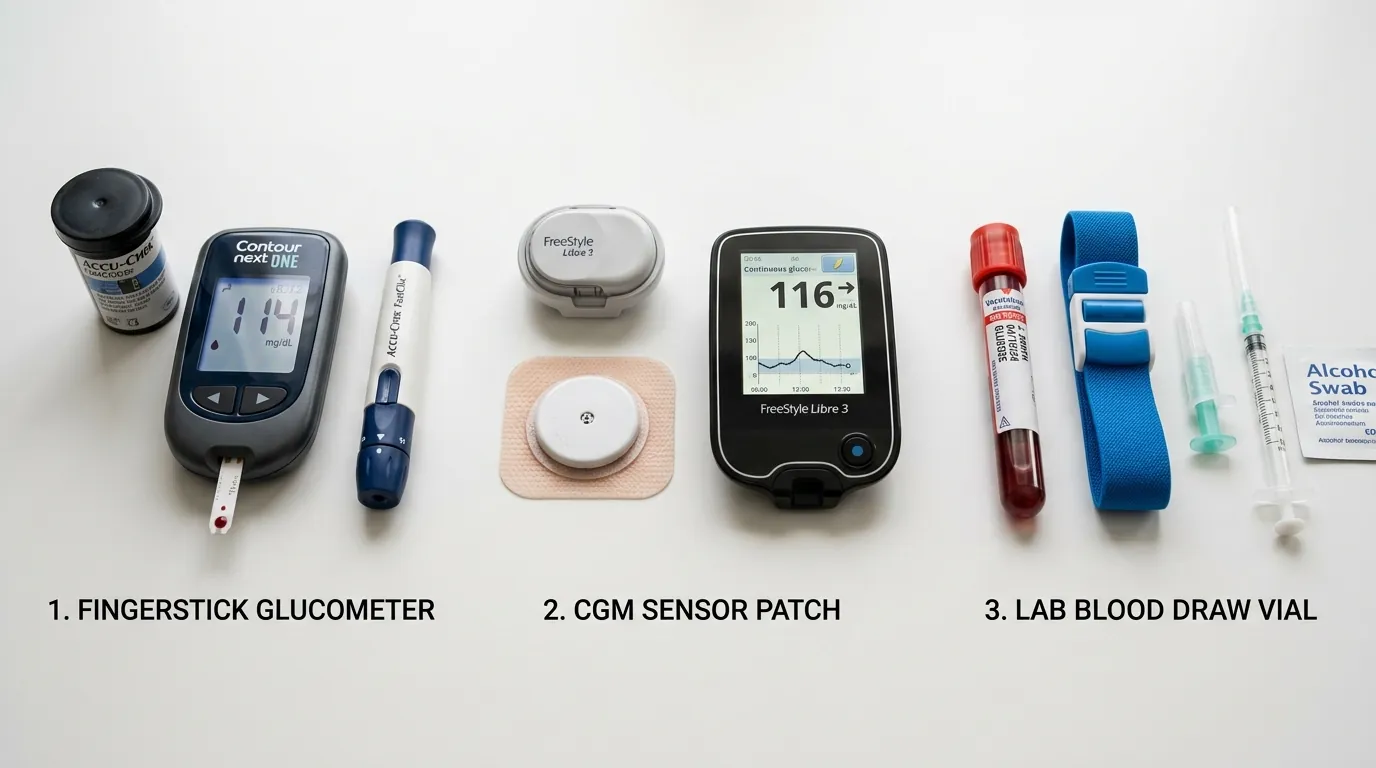
Five primary technologies exist for measuring blood glucose, each providing a fundamentally different type of information. Continuous glucose monitors (CGMs) measure interstitial fluid glucose every 1 to 5 minutes, producing 288 to 1,440 data points per day with a MARD of 7.9 to 9.1%. Self-monitoring blood glucose (SMBG) meters use a fingerstick capillary blood sample to provide a single glucose reading with FDA-allowed accuracy of plus or minus 15%. Laboratory fasting plasma glucose tests draw venous blood after 8+ hours of fasting and measure glucose with reference-grade accuracy (coefficient of variation less than 3%). The A1C test measures glycated hemoglobin in a venous blood sample, reflecting average glucose over 2 to 3 months. The oral glucose tolerance test (OGTT) measures glucose at baseline and 2 hours after ingesting a 75-gram glucose solution, serving as the gold standard for diagnosing gestational diabetes and impaired glucose tolerance. Each test answers a different clinical question: CGMs answer "what is my glucose doing right now and what pattern does it follow?" SMBG answers "what is my glucose at this exact moment?" Fasting glucose answers "what is my baseline glucose?" A1C answers "what has my average glucose been?" OGTT answers "how efficiently does my body process a glucose load?"
Continuous Glucose Monitors: 288 Daily Readings
A continuous glucose monitor is a wearable sensor that measures glucose in interstitial fluid every 1 to 5 minutes and transmits readings via Bluetooth to a smartphone or receiver. The Dexcom G7 takes readings every 5 minutes (288 per day) with a MARD of 8.2%. The FreeStyle Libre 3 measures every minute (1,440 per day) with a MARD of 7.9%. The Eversense E3 implantable sensor measures every 5 minutes with a MARD of 8.5% and lasts 180 days. Monthly costs range from $75 for subscription-model OTC devices (Dexcom Stelo, Abbott Lingo) to $300 or more for prescription CGMs without insurance. With insurance, most patients pay $0 to $75 per month. CGMs provide unique clinical data that no other testing method can: Time in Range, Time Below Range, Time Above Range, glucose variability (coefficient of variation), Glucose Management Indicator, overnight glucose profiles, postmeal response curves, and predictive high/low glucose alerts. The 2017 DIAMOND trial demonstrated that CGM use reduced A1C by 0.6% more than SMBG alone, and the 2020 MOBILE trial (Martens et al., JAMA) showed that CGMs reduced A1C by 0.4% and Time Below Range by 50% in type 2 diabetes patients on basal insulin. These outcomes data have led the ADA to recommend CGM for all insulin-treated patients and to recognize its value in non-insulin-treated type 2 diabetes and prediabetes.
Fingerstick Blood Glucose Meters
Self-monitoring blood glucose (SMBG) meters measure capillary blood glucose from a fingertip lancet prick. The user places a small blood drop (0.3 to 1.0 microliters) on a disposable test strip containing glucose oxidase enzyme; the strip generates an electrochemical signal proportional to the glucose concentration, and the meter displays the result in 3 to 5 seconds. FDA requirements for SMBG meters mandate that 95% of readings must fall within plus or minus 15 mg/dL (for glucose below 75 mg/dL) or plus or minus 15% (for glucose at or above 75 mg/dL) of a laboratory reference. Typical users perform 4 to 10 tests per day: before meals, 2 hours after meals, at bedtime, and when symptoms suggest hypo- or hyperglycemia. Test strip costs range from $0.20 to $1.50 per strip, totaling $15 to $75 per month for 4 to 10 daily tests. SMBG has been the standard of care for diabetes self-management since the 1980s, but it provides only isolated snapshots — it cannot detect overnight glucose patterns, postmeal response curves, glucose variability, or the rate and direction of glucose change. A fingerstick reading of 110 mg/dL could represent stable glucose or the midpoint of a rapid fall from 200 mg/dL — information that only CGM trend arrows can distinguish. Despite these limitations, fingerstick meters remain essential for CGM calibration verification, confirming CGM readings during rapid glucose changes, and as a backup when CGM sensors fail.
Laboratory Tests: Fasting Glucose, A1C, and OGTT
Laboratory blood tests provide the highest accuracy and serve as the diagnostic standard for diabetes classification. Fasting plasma glucose (FPG) is measured from a venous blood draw after 8+ hours of fasting, analyzed by automated chemistry analyzers with a coefficient of variation below 3%. The test costs $15 to $100 depending on insurance and laboratory. FPG below 100 mg/dL is normal, 100-125 mg/dL indicates prediabetes, and 126 mg/dL or higher on two separate tests confirms diabetes. The A1C test measures the fraction of glycated hemoglobin using high-performance liquid chromatography (HPLC) or immunoassay, with a coefficient of variation below 5%. It costs $25 to $50 and is recommended every 3 months for people with diabetes and annually for screening in adults over 45 or those with risk factors. The oral glucose tolerance test (OGTT) is the most labor-intensive: the patient fasts overnight, a baseline blood draw is taken, the patient drinks a 75-gram glucose solution, and blood glucose is measured at 1 hour and 2 hours post-ingestion. Normal 2-hour glucose is below 140 mg/dL; 140-199 indicates impaired glucose tolerance (prediabetes); 200 or above confirms diabetes. The OGTT costs $50 to $150 and requires 2 to 3 hours in a clinical setting. It is the preferred diagnostic test for gestational diabetes (using the 50-gram glucose challenge test as the first screen) and is the most sensitive test for detecting impaired glucose tolerance that fasting glucose and A1C may miss.
Choosing the Right Testing Method for Your Situation
The optimal blood sugar testing method depends on the clinical context, diagnosis, treatment regimen, and individual goals. For type 1 diabetes, CGM is the standard of care recommended by the ADA, the Endocrine Society, and the International Society for Pediatric and Adolescent Diabetes (ISPAD) — fingerstick meters serve as backup and calibration verification only. For type 2 diabetes on insulin therapy, CGM is recommended by the ADA based on the MOBILE trial evidence showing 0.4% A1C improvement and significant hypoglycemia reduction. For type 2 diabetes managed with oral medications, CGM provides benefit for identifying postmeal spikes and optimizing diet, though insurance coverage varies — OTC devices ($75 per month) are an accessible option. For prediabetes, OTC CGMs (Dexcom Stelo, Abbott Lingo) provide actionable data for identifying personal glucose triggers and measuring the impact of lifestyle changes, combined with quarterly A1C tests to track progress. For gestational diabetes, intensive monitoring is required: CGM or 4 to 7 daily fingerstick tests during pregnancy, with OGTT at 24-28 weeks for diagnosis. For general wellness and metabolic optimization, an OTC CGM trial of 1 to 3 months provides insight into personal glucose responses that inform long-term dietary and lifestyle choices. Lab fasting glucose and A1C remain essential for initial diagnosis regardless of CGM use.