Blood Sugar After Eating: 1-Hour and 2-Hour Postprandial Targets
Postprandial glucose should peak below 180 mg/dL at 1 hour and return below 140 mg/dL at 2 hours. How meal composition, eating order, and CGM data reveal your personal glucose response.
What Happens to Blood Sugar After You Eat
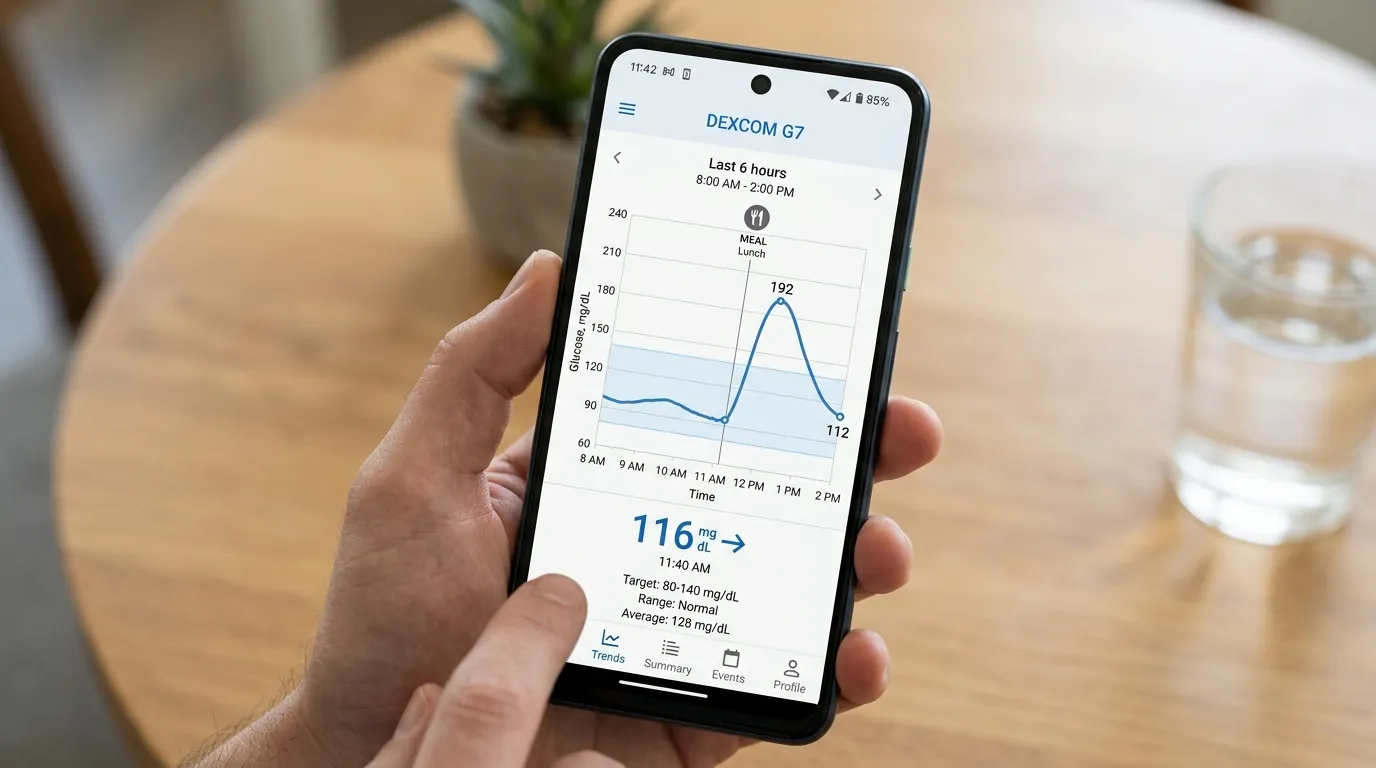
Blood sugar begins rising within 10 to 15 minutes of the first bite of food as simple sugars are absorbed through the small intestine into the portal vein and then into systemic circulation. The glucose response curve follows a predictable pattern: a rise phase (15-60 minutes), a peak phase (30-90 minutes depending on meal composition), and a return-to-baseline phase (90-180 minutes). In a non-diabetic adult, the peak postmeal glucose typically reaches 120 to 160 mg/dL and returns below 140 mg/dL within 2 hours. The American Diabetes Association defines normal postprandial glucose as below 140 mg/dL at the 2-hour mark. For people with diabetes, the target is below 180 mg/dL at 1 to 2 hours after the start of the meal. The magnitude of the postmeal spike is determined primarily by three factors: the total grams of carbohydrates consumed, the glycemic index of those carbohydrates, and the presence of fiber, fat, and protein that slow gastric emptying. A meal of 60 grams of white rice alone produces a peak glucose of 180 to 220 mg/dL in a healthy adult, while the same 60 grams of rice eaten with 30 grams of protein and 15 grams of fat produces a peak of 130 to 160 mg/dL — a 30 to 40% reduction in spike height.
Postprandial Glucose Targets: ADA and International Standards
The ADA 2024 Standards of Care recommend a postprandial glucose target of less than 180 mg/dL for most adults with diabetes, measured 1 to 2 hours after the start of the meal. The International Diabetes Federation (IDF) recommends a tighter target of less than 160 mg/dL at 1 hour for people pursuing optimal glycemic control. For pregnancy, the targets are significantly stricter: less than 140 mg/dL at 1 hour and less than 120 mg/dL at 2 hours. The 2019 International Consensus on Time in Range established that 70-180 mg/dL is the standard glucose range for calculating TIR, with less than 25% of time above 180 mg/dL as the target for type 1 and type 2 diabetes and less than 5% of time above 250 mg/dL. Non-diabetic adults pursuing metabolic optimization through over-the-counter CGMs often aim for even tighter targets — keeping postmeal glucose below 140 mg/dL and limiting excursions above 120 mg/dL to fewer than 3 per day. A 2020 Virta Health analysis of 14,000 CGM users found that postmeal glucose peaks were the strongest predictor of daily time in range, accounting for 68% of the variance in TIR across the study population.
How Meal Composition Affects Postmeal Glucose
The macronutrient composition of a meal is the primary determinant of the postprandial glucose response curve — more impactful than total calories, portion size, or glycemic index alone. Carbohydrates raise blood sugar directly because they are digested into glucose. Proteins have a modest glucose-raising effect (approximately 50% of protein grams are converted to glucose through gluconeogenesis, but this process takes 3 to 5 hours). Fats do not raise blood sugar directly but slow gastric emptying, which spreads the carbohydrate absorption over a longer time window and reduces peak glucose. Fiber — particularly viscous soluble fiber from oats, beans, and psyllium — creates a gel in the small intestine that physically slows glucose absorption. A 2019 meta-analysis in Diabetes Care (Reynolds et al.) covering 185 prospective studies found that each additional 8 grams of dietary fiber per day reduced the risk of type 2 diabetes by 15%. The practical implication for postmeal glucose management: pairing carbohydrates with at least 20 grams of protein and 10 grams of fat reduces the postmeal spike by 30 to 50% compared to eating the same carbohydrates alone. CGM users can verify this effect in real time by comparing the glucose curves of identical carbohydrate portions consumed with and without protein and fat.
The Meal Order Effect: Why Eating Vegetables First Matters
The order in which you eat foods within a meal significantly affects the postmeal glucose response — a finding with profound practical implications for blood sugar management. A landmark 2015 study at Weill Cornell Medical College (Shukla et al., Diabetes Care) measured postmeal glucose in 11 adults with type 2 diabetes who ate the same meal in two different orders: carbohydrates first (bread and orange juice) followed by protein, fat, and vegetables, versus vegetables and protein first followed by carbohydrates. Eating vegetables and protein before carbohydrates reduced the postmeal glucose peak by 73% and the insulin peak by 48%. A follow-up study by the same team in 2019 (BMJ Open Diabetes Research and Care) confirmed the effect in a larger sample and found that the glucose-lowering benefit persisted for at least 3 hours. The mechanism is straightforward: protein and fiber in the stomach slow gastric emptying, and the incretin hormones GLP-1 and GIP released in response to protein slow carbohydrate absorption in the small intestine. This meal order strategy is now one of the most recommended CGM-informed dietary interventions, because the effect is immediately visible as a flatter, lower glucose curve on the continuous glucose monitor display.
CGM Data and Personal Postmeal Glucose Responses
One of the most significant findings in metabolic research is that postmeal glucose responses are highly personalized — two people eating identical meals can have glucose spikes that differ by 40 to 80 mg/dL. This was definitively demonstrated by the Weizmann Institute Personalized Nutrition Project (Zeevi et al., Cell, 2015), which placed CGMs on 800 participants and measured their glucose responses to 46,898 meals. The study found that individual responses to identical foods varied so widely that population-level glycemic index values were poor predictors of personal glucose spikes. For example, some participants spiked more from bananas than from cookies, while others showed the opposite pattern. The gut microbiome composition, meal timing, sleep history, physical activity in the preceding 24 hours, and genetic variants in glucose transporter genes all contributed to this variability. These findings established the scientific foundation for personalized nutrition guided by CGM data. Over-the-counter CGMs now enable any individual to identify their personal glucose triggers — the specific foods, portions, and meal times that produce the highest spikes — and adjust their diet based on objective data rather than generalized dietary guidelines.