A white bread sandwich spikes one person's blood sugar to 167 mg/dL and another person's to 108 mg/dL. This is not a measurement error—it is the central finding of personalized nutrition research that has fundamentally changed how scientists understand glucose metabolism. The glycemic index, long treated as a universal food property, is actually a population average that obscures enormous individual variation.
The Weizmann Institute Study That Changed Everything
In 2015 researchers at the Weizmann Institute of Science in Israel published a landmark study in the journal Cell. The study enrolled 800 participants who wore continuous glucose monitors for 1 week while eating 46,898 standardized meals. The results demolished the assumption that foods have a fixed glycemic effect.
**Key finding: individual glucose responses to identical foods varied by up to 60 percent.** Some participants spiked higher on bananas than on cookies; others showed the reverse. The correlation between a food's published glycemic index and an individual's actual glucose response was weak—an R-squared of only 0.38, meaning the glycemic index explained less than 40 percent of the variability in personal glucose responses.
The researchers built a machine learning algorithm that predicted individual glucose responses with significantly better accuracy than the glycemic index alone. The algorithm incorporated 137 variables, including gut microbiome composition, meal timing, recent physical activity, sleep duration, and body composition.
The Gut Microbiome: Your Personal Glucose Filter
The Weizmann team identified the gut microbiome as the single most important predictor of individual glucose responses after accounting for the meal itself. Each person harbors approximately 38 trillion bacteria in their gastrointestinal tract, and the composition of these microbial communities varies dramatically between individuals.
Specific bacterial species influence glucose metabolism through multiple mechanisms:
**Short-chain fatty acid production.** Bacteria like Akkermansia muciniphila and various Bifidobacterium species ferment dietary fiber into short-chain fatty acids (butyrate, propionate, acetate), which improve insulin sensitivity and slow glucose absorption. People with higher populations of these bacteria show flatter glucose curves after carbohydrate-rich meals.
**Bile acid modification.** Gut bacteria transform primary bile acids into secondary forms that activate the FXR and TGR5 receptors, which regulate glucose homeostasis. Variations in bile acid profiles—driven by microbiome composition—explain part of the inter-individual difference in glucose responses to fat-containing meals.
**Mucosal barrier integrity.** A healthy microbiome maintains the intestinal mucosal barrier, preventing bacterial endotoxins (lipopolysaccharides) from leaking into the bloodstream. Endotoxin exposure triggers low-grade inflammation that impairs insulin signaling. People with compromised gut barriers often show elevated and prolonged glucose responses.
Genetics: The Hardware Layer
While the microbiome acts as modifiable software, genetics provides the hardware baseline. Research from the Stanford iPOP (Integrated Personal Omics Profiling) study and the PREDICT study (published in Nature Medicine, 2020) identified several genetic factors that influence glucose responses:
**Insulin secretion capacity.** Variants in the TCF7L2 gene—the strongest genetic risk factor for type 2 diabetes—affect how quickly and how much insulin the pancreas releases after a glucose load. People with the risk variant secrete insulin more slowly, leading to higher post-meal glucose peaks.
**GLUT4 transporter density.** Genetic variations affecting the expression of GLUT4 glucose transporters in muscle tissue determine how efficiently muscles absorb glucose from the bloodstream. Higher GLUT4 expression means faster glucose clearance after meals.
**Amylase gene copies.** The AMY1 gene encodes salivary amylase, the enzyme that begins starch digestion in the mouth. Humans carry between 2 and 18 copies of AMY1, and people with more copies digest starch faster—producing earlier and sometimes higher glucose spikes from starchy foods. A 2023 study in Nature Genetics confirmed that AMY1 copy number significantly predicts the glucose response to bread and rice.
The PREDICT Studies: Twins Diverge
The PREDICT 1 study (King's College London, published in Nature Medicine 2020) enrolled 1,002 participants—including 240 identical twins—and measured glucose, insulin, and triglyceride responses to standardized meals. Even identical twins, who share 100 percent of their DNA, showed only 37 percent concordance in their glucose responses to the same meals. The remaining 63 percent of the variation was attributed to non-genetic factors: microbiome composition, sleep, meal timing, exercise habits, and stress.
**This finding proved that genetics alone does not determine glucose responses.** Environmental and behavioral factors account for the majority of inter-individual variation, which means glucose responses are modifiable through lifestyle changes.
What This Means for CGM Users
The practical implication is straightforward: **population-level dietary advice (eat this, avoid that) cannot account for individual glucose biology.** A food that is "healthy" by glycemic index standards may produce an unhealthy glucose response in a specific person, and vice versa.
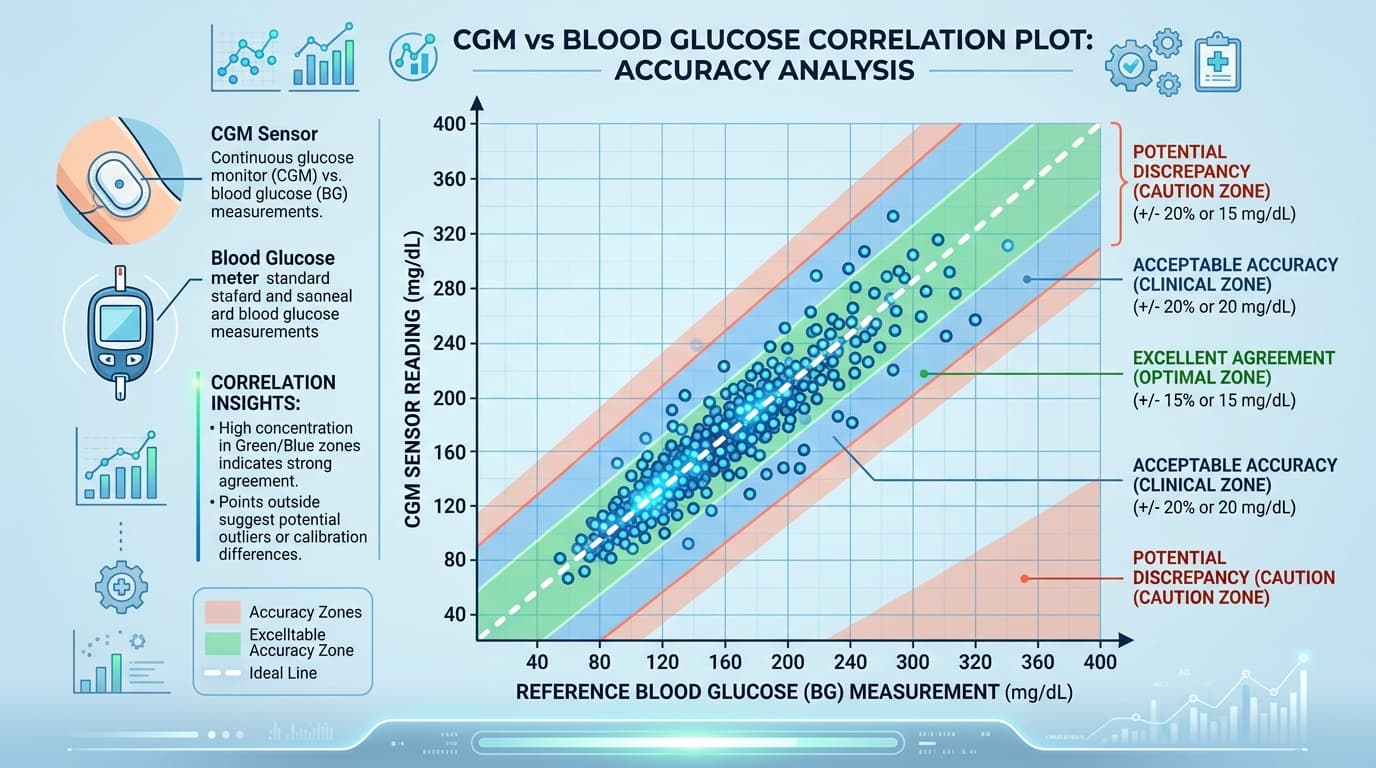
A continuous glucose monitor is the only consumer tool that captures individual glucose responses in real time. Two weeks of CGM data—testing your regular meals and tracking the glucose response to each—produces a personalized nutrition map that no dietary guideline, glycemic index table, or generic meal plan can replicate.
The OTC CGM market makes this accessible without a prescription. Both Dexcom Stelo and Abbott Lingo provide the accuracy needed to distinguish meaningful differences in meal responses. For a detailed comparison, our CGM comparison guides cover accuracy (MARD), pricing, and app features across all major devices.
The Future: Personalized Nutrition at Scale
The convergence of CGM data, microbiome testing, and machine learning is creating a new paradigm in nutrition science. Companies like DayTwo (acquired by Ypsomed), Zoe, and January AI are building platforms that combine CGM readings with gut microbiome sequencing to predict glucose responses before a person eats. Early results from Zoe's PREDICT 3 study show that personalized meal recommendations based on microbiome and CGM data reduced post-meal glucose spikes by 30 percent compared to generic dietary advice.
The era of one-size-fits-all nutrition is ending. The data is clear: your glucose response is yours alone, shaped by a unique combination of genetics, microbiome, lifestyle, and metabolic history. A CGM makes that individuality visible for the first time.