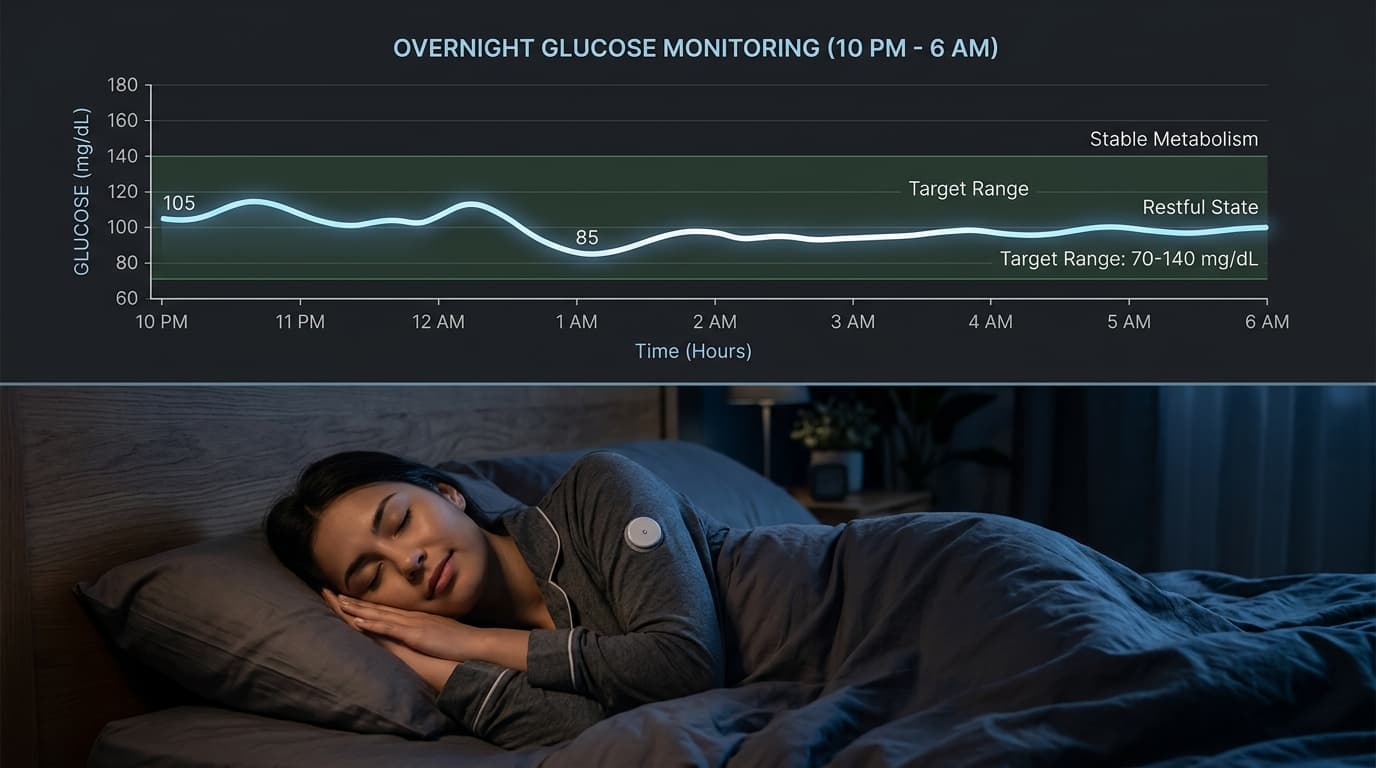
One of the most revealing uses of a continuous glucose monitor happens while you sleep. The 8 hours you spend in bed generate roughly 96 glucose readings on a CGM sensor, and those nighttime data points tell a story that daytime monitoring alone cannot capture. Research increasingly shows that the relationship between glucose and sleep runs in both directions: unstable blood sugar disrupts sleep quality, and poor sleep worsens glucose control.
What Normal Overnight Glucose Looks Like
In a metabolically healthy adult, overnight glucose follows a predictable pattern. After dinner, blood sugar rises to a post-meal peak (typically below 140 mg/dL), then gradually declines over 2-3 hours to a baseline fasting level. During the first half of the night, glucose stabilizes in the 70-90 mg/dL range and remains relatively flat.
Between 4 and 8 AM, a natural rise of 10-20 mg/dL occurs as the body prepares for waking. This rise—driven by cortisol, growth hormone, and glucagon—is called the dawn phenomenon. In healthy individuals, the fasting glucose upon waking still falls below 100 mg/dL.
Nocturnal Hypoglycemia: The Hidden Danger
For people with diabetes who use insulin or sulfonylureas, nocturnal hypoglycemia (glucose below 70 mg/dL during sleep) is a serious risk. Studies estimate that 50 percent of all severe hypoglycemic episodes occur during sleep, and most go undetected without a CGM because the person does not wake up.
Symptoms of nocturnal low blood sugar include night sweats, restless sleep, nightmares, morning headaches, and fatigue upon waking. A continuous glucose monitor with low-glucose alarms—available on Dexcom G7, Libre 3, and Medtronic Guardian 4—can wake the user or alert a caregiver when glucose drops below a set threshold (commonly 70 or 55 mg/dL).
How Late-Night Eating Affects Your CGM Data
CGM data reveals a consistent pattern among late-night eaters: meals consumed within 2 hours of bedtime produce glucose elevations that persist into the first sleep cycle, raising average overnight glucose and increasing glucose variability. A 2022 study in the journal Nutrients found that participants who ate their last meal 4 or more hours before bedtime had 18 percent lower overnight glucose variability compared to those who ate within 2 hours of sleep.
The composition of the late meal matters as much as timing. A high-carbohydrate snack before bed produces a sharp spike followed by a reactive dip, which can trigger a cortisol response and disrupt deep sleep. A protein-and-fat-focused snack (such as nuts, cheese, or Greek yogurt) produces a more gradual, lower-amplitude glucose curve that is less likely to interfere with sleep architecture.
Poor Sleep Worsens Glucose Control
The relationship is bidirectional. A single night of restricted sleep (4-5 hours) reduces insulin sensitivity by 25-30 percent the following day, according to research published in the Annals of Internal Medicine. CGM data from sleep-deprived individuals shows higher post-meal glucose spikes, slower glucose clearance, and elevated fasting glucose the morning after a short night.
Chronic sleep restriction—sleeping fewer than 6 hours per night—is associated with a 1.5 to 2-fold increased risk of developing type 2 diabetes, independent of diet and exercise. For people already managing diabetes, improving sleep duration and quality can measurably improve time in range on their CGM.
Practical Tips from CGM Night Data
After wearing a CGM for 2-3 weeks, review your overnight glucose trends and look for these patterns:
- **Flat and low (70-90 mg/dL):** Ideal. Your overnight metabolism is well regulated. - **Elevated baseline (100-120 mg/dL):** May indicate insulin resistance or late-night eating. Try moving dinner earlier. - **Nocturnal dips below 70 mg/dL:** Discuss with your physician—medication timing or dosing may need adjustment. - **Large dawn phenomenon (rise of 30+ mg/dL):** Common in type 2 diabetes. Exercise in the evening may blunt the morning rise.
The glucose-sleep connection is one of the most actionable insights a continuous glucose monitor provides. Small changes—eating dinner earlier, maintaining consistent bedtimes, and addressing sleep apnea—can produce measurable improvements visible in your next AGP report.